Minimally Invasive Total Hip Replacement
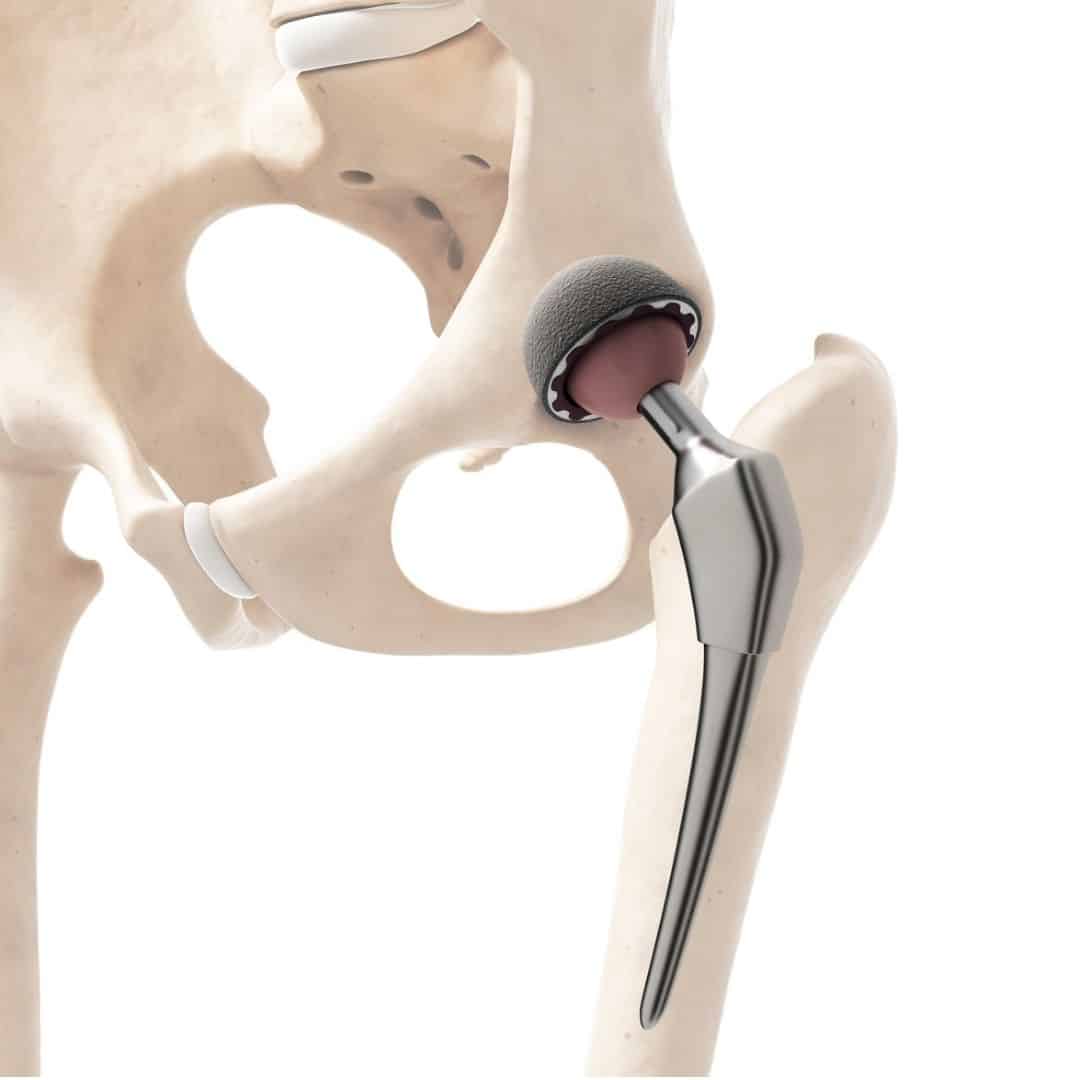
The hip joint is one of the body's largest weight-bearing joints and is the point where the thigh bone (femur) and the pelvis (acetabulum) join. It is a ball and socket joint in which the head of the femur is the ball and the pelvic acetabulum forms the socket. The joint surface is covered by a smooth articular cartilage that cushions and enables smooth movements of the joint.
Hip arthritis is one of the painful and common diseases of the hip joint caused by damage to the cartilage. Total hip replacement surgery is an option to relieve severe arthritis pain that limits your daily activities.
Traditionally, a total hip replacement will be performed through a 10–12-inch-long incision made on the side of the hip. A minimally invasive approach has been developed in recent years where surgery is performed through one or two smaller incisions rather than the single long incision as in the traditional approach. Advantages of the newer approach are lesser muscle dissection, minimal pain, quicker recovery, and faster rehabilitation.
Arthritis is inflammation of the joints resulting in pain, swelling, stiffness, and limited movement. Hip arthritis is a common cause of chronic hip pain and disability. The most common type of arthritis affecting the hip is osteoarthritis which is characterized by progressive wearing away of the joint cartilage. As the protective cartilage wears down, the bone ends rub against each other and cause pain in the hip. It is more common in individuals aged above 50 years and tends to run in families.
Symptoms
The most common symptom of hip arthritis is dull, aching joint pain and stiffness resulting in limited mobility. There may be pain in the groin, thigh, and buttock area and sometimes pain may be referred to as the knee. Vigorous activity and walking for long distances can increase pain and stiffness which may cause limping while walking.
Diagnosis
Diagnosis is made by evaluating your symptoms, medical history, physical examination, and X-rays. Sometimes, additional imaging tests such as MRI and CT scans may be needed to confirm the diagnosis.
Surgical procedure
Surgery may be recommended in patients with severe cartilage damage and if conservative treatment options such as anti-inflammatory medications and physical therapy do not relieve the symptoms.
For minimally invasive hip replacement, the surgical technique and artificial implants remain the same as a traditional hip replacement however the difference is smaller incisions and minimal soft tissue dissection. The surgery is performed through either one or two smaller incisions. The procedure is performed under general anesthesia.
A single incision minimally invasive approach, your surgeon makes a 3–6-inch incision over the side of the hip to expose the hip joint. The muscles are minimally dissected to reach the joint. The femur is dislocated from the acetabulum. The surface of the socket is cleaned and the arthritic bone is removed using a reamer. The acetabular implant is inserted into the socket using screws or special cement. A liner material of plastic, ceramic, or metal is placed inside the acetabular component. The femur or thigh bone is then prepared by removing the arthritic bone using special instruments and shaped to exactly fit the new metal femoral component. The femoral stem is then inserted into the femur either by a press fit or using bone cement. Then the femoral head component made of metal or ceramic is placed on the femoral stem. All the new parts are secured in place using special cement. The muscles and tendons around the new joint are repaired and the incision is closed.
If the surgeon uses the two-incision technique, a 2- to 3-inch incision is made over the groin for placement of the socket, and a 1- to 2-inch incision is made over the buttock for placement of the femoral stem. This technique requires a longer operative time and is performed under X-ray guidance.
Advantages
The advantages of minimally invasive total hip replacement as compared with traditional total hip replacement may include:
- Smaller incisions
- Shorter hospital stay
- Less trauma to the surrounding tissues
- Quicker recovery
- Less blood loss
- Less scarring
- Faster rehabilitation
- Minimal post-operative pain
AFTER SURGERY
After surgery, you will feel pain. This is completely normal and part of the healing process. Your doctor and nurses will work together to reduce your pain, this will help you recover faster.
Prior to you leaving the hospital your doctor will send a prescription to your pharmacy for some short-term pain relief after surgery. Your doctor may suggest multiple medications to help manage your pain, such as opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor will discuss which options or combinations would be best for you.
OPIOIDS
At MD West One, your health is always a top priority, which is why we are very passionate about getting you back to full activity in a safe and timely manner. We understand every patient is unique when it comes to pain management. A key component of a successful pain treatment plan includes weighing all risks and benefits to find the pain treatment plan that best fits you.
A high risk of dependence and overdose is associated with the use of opioids. To avoid this from accruing our agreement with you:
- You should take all medications as ordered by your provider. If you take the medication in excess of what is prescribed and run out of the medication prior to the refill date, the refill will not be authorized early.
- If you are requiring a refill of your prescription please call during regular business hours. Our providers will not refill any pain medications over the weekend, holidays, or after clinic hours.
- Make sure to tell your physician or nurse which medications you are taking, including herbal remedies, since narcotic medications can interact with over-the-counter medications and other prescribed medications, especially cough syrups that contain alcohol, codeine, or hydrocodone.
- Alteration of any written prescription, sharing, trading, or selling your medication is a federal offense and will be reported.
- You are responsible for keeping your pain medication in a safe and secure place, such as a locked cabinet or safe. Stolen medications should be reported to the police and to your physician immediately.
- If your medications are lost, misplaced, or stolen, your physician may choose not to replace the medications or to taper and discontinue the medications.
Post-operative precautions
After undergoing minimally invasive total hip replacement, you must take special care to prevent dislocation of the new joint and to ensure proper healing.
- Avoid combined movement of bending your hip and turning your foot inwards
- Keep a pillow between your legs while sleeping for 6 weeks
- Never cross your legs and bend your hips past a right angle (90°)
- Avoid sitting on low chairs
- Avoid bending down to pick up things, instead use a grabber device.
- Use an elevated toilet seat
Risk Factors
As with any major surgical procedure, there are certain potential risks and complications involved with total hip replacement surgery. They include:
- Infection
- Injury to nerves and blood vessels
- Formation of blood clots in the leg veins
- Implant malposition
- Fracture of the femur or pelvis
Don't wait any longer to get relief. Make an appointment to see one of our orthopedic specialists.
AMERICAN ACADEMY OF ORTHOPEDIC SURGEONS
This article has been written and peer-reviewed by the American Academy of Orthopaedic Surgeons.
