Total Knee Replacement
Total knee replacement, also called total knee arthroplasty, is a surgical procedure in which the worn out or damaged surfaces of the knee joint are removed and replaced with artificial parts. The knee is made up of the femur (thigh bone), the tibia (shin bone), and the patella (kneecap). The meniscus, the soft cartilage between the femur and tibia, serves as a cushion and helps absorb shock during motion. Arthritis (inflammation of the joints), injury, or other diseases of the joint can damage this protective layer of cartilage, causing extreme pain and difficulty in performing daily activities. Your doctor may recommend surgery if non-surgical treatment options have failed to relieve the symptoms.
Your doctor may advise total knee replacement if you have:
- Severe knee pain that limits your daily activities (such as walking, getting up from a chair, or climbing stairs).
- Moderate to severe pain that occurs during rest or awakens you at night.
- Chronic knee inflammation and swelling that is not relieved with rest or medications
- Failure to obtain pain relief from medications, injections, physical therapy, or other conservative treatments.
- A bow-legged knee deformity
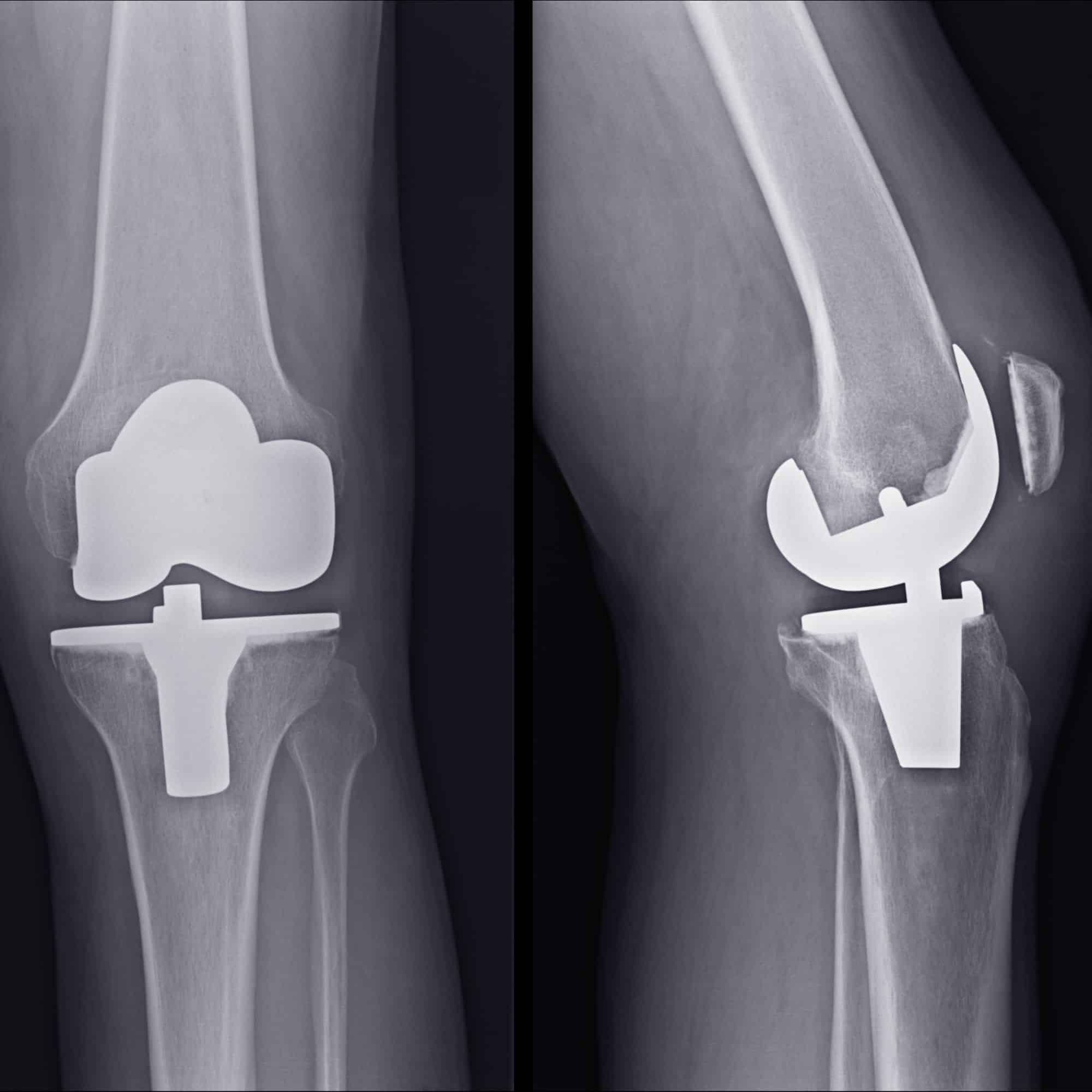
Indications
Total knee replacement surgery is commonly indicated for severe osteoarthritis of the knee. Osteoarthritis is the most common form of knee arthritis in which the joint cartilage gradually wears away. It often affects older people.
In a normal joint, articular cartilage allows for smooth movement within the joint, whereas in an arthritic knee the cartilage itself becomes thinner or completely absent. In addition, the bones become thicker around the edges of the joint and may form bony “spurs”. These factors can cause pain and restricted range of motion in the joint.
Causes
The exact cause of osteoarthritis is not known, however, there are several factors that are commonly associated with the onset of arthritis and may include:
- Injury or trauma to the joint
- Fractures at the knee joint
- Increased body weight
- Repetitive overuse
- Joint infection
- Inflammation of the joint
- Connective tissue disorders
Diagnosis
Your doctor will diagnose osteoarthritis based on the medical history, physical examination, and X-rays. X-rays typically show a narrowing of the joint space in the arthritic knee.
Procedure
The goal of total knee replacement surgery is to relieve pain and restore the alignment and function of your knee.
The surgery is performed under spinal or general anesthesia. Your surgeon will make an incision in the skin over the affected knee to expose the knee joint. Then the damaged portions of the femur bone are cut at appropriate angles using specialized jigs. The femoral component is attached to the end of the femur with or without bone cement. The surgeon then cuts or shaves the damaged area of the tibia (shinbone) and the cartilage. This removes the deformed part of the bone and any bony growths, as well as creates a smooth surface on which the implants can be attached. Next, the tibial component is secured to the end of the bone with bone cement or screws. Your surgeon will place a plastic piece called an articular surface between the implants to provide a smooth gliding surface for movement. This plastic insert will support the body’s weight and allow the femur to move over the tibia, like the original meniscus cartilage. The femur and the tibia with the new components are then put together to form the new knee joint. To make sure the patella (knee cap) glides smoothly over the new artificial knee, its rear surface is also prepared to receive a plastic component. With all the new components in place, the knee joint is tested through its range of motion. The entire joint is then irrigated and cleaned with a sterile solution. The incision is carefully closed; drains are inserted and a sterile dressing is placed over the incision.
AFTER SURGERY
After surgery, you will feel pain. This is completely normal and part of the healing process. Your doctor and nurses will work together to reduce your pain, this will help you recover faster.
Prior to you leaving the hospital your doctor will send a prescription to your pharmacy for some short-term pain relief after surgery. Your doctor may suggest multiple medications to help manage your pain, such as opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor will discuss which options or combinations would be best for you.
OPIOIDS
At MD West One, your health is always a top priority, which is why we are very passionate about getting you back to full activity in a safe and timely manner. We understand every patient is unique when it comes to pain management. A key component of a successful pain treatment plan includes weighing all risks and benefits to find the pain treatment plan that best fits you.
A high risk of dependence and overdose is associated with the use of opioids. To avoid this from accruing our agreement with you:
- You should take all medications as ordered by your provider. If you take the medication in excess of what is prescribed and run out of the medication prior to the refill date, the refill will not be authorized early.
- If you are requiring a refill of your prescription please call during regular business hours. Our providers will not refill any pain medications over the weekend, holidays, or after clinic hours.
- Make sure to tell your physician or nurse which medications you are taking, including herbal remedies, since narcotic medications can interact with over-the-counter medications and other prescribed medications, especially cough syrups that contain alcohol, codeine, or hydrocodone.
- Alteration of any written prescription, sharing, trading, or selling your medication is a federal offense and will be reported.
- You are responsible for keeping your pain medication in a safe and secure place, such as a locked cabinet or safe. Stolen medications should be reported to the police and to your physician immediately.
- If your medications are lost, misplaced, or stolen, your physician may choose not to replace the medications or to taper and discontinue the medications.
Post-operative care
Rehabilitation begins immediately following the surgery. A physical therapist will teach you specific exercises to strengthen your leg and restore knee movement. Knee immobilizers are used to stabilize the knee. You will be able to walk with crutches or a walker. A continuous passive motion (CPM) machine can be used to move the knee joint. Continuous passive motion is a device attached to the treated leg which constantly moves the joint through a controlled range of motion, while the patient relaxes. Your physical therapist will also provide you with a home exercise program to strengthen your thigh and calf muscles.
Risks and complications
As with any major surgery, possible risks and complications associated with total knee replacement surgery include:
- Knee stiffness
- Infection
- Blood clots (deep vein thrombosis)
- Nerve and blood vessel damage
- Ligament injuries
- Patella (kneecap) dislocation
- Plastic liner wears out
- Loosening of the implant
If you find difficulty in performing simple activities such as walking or climbing stairs because of your severe arthritic knee pain, then total knee replacement may be an option for you. It is a safe and effective procedure to relieve pain, correct leg deformity, and help you resume your normal activities of daily living
Don't wait any longer to get relief. Make an appointment to see one of our orthopedic specialists.
AMERICAN ASSOCIATION OF HIP and KNEE SURGEONS
This article has been written and peer-reviewed by the AAHKS Patient and Public Relations Committee and the AAHKS Evidence-Based Medicine Committee.
